Spotting Meningitis: Key Symptoms & Why Early Action Matters
Meningitis is a word that immediately evokes a sense of urgency and concern for good reason. Understanding its meaning – what we refer to in Dutch as
Meningitis Betekenis – is the first crucial step in protecting ourselves and our loved ones from its devastating potential. At its core, meningitis signifies an inflammation of the meninges, the protective membranes that surround the brain and spinal cord, as well as the cerebrospinal fluid that bathes them. This serious condition, often referred to as "nekkramp" in some regions, demands immediate attention due to its rapid onset and potential for severe, life-altering complications or even fatality if not diagnosed and treated promptly.
Whether caused by bacteria, viruses, or, more rarely, fungi, the body's response to infection in such a critical area can lead to a cascade of symptoms that, while sometimes mirroring common illnesses, should never be ignored. This article will delve into the critical symptoms of meningitis, explore its various causes, and underscore the profound importance of seeking swift medical intervention.
Unpacking the Causes: What Triggers Meningitis?
Meningitis isn't a single disease but rather a condition that can arise from a variety of sources. Knowing the underlying cause is paramount for effective treatment. While the reference context highlights several, it’s beneficial to understand their distinct characteristics.
Meningitis Causes: Understanding Bacterial, Viral, and Prevention elaborates further on these distinctions.
Bacterial Meningitis: The Most Severe Form
Considered the most dangerous type, bacterial meningitis is a medical emergency. It often develops rapidly and can be life-threatening. Common culprits include:
*
Streptococcus pneumoniae (Pneumococcus): A frequent cause, responsible for a significant percentage of bacterial meningitis cases. These bacteria can reside harmlessly in the nose and throat but can cause serious infection if they enter the bloodstream and spread to the meninges.
*
Neisseria meningitidis (Meningococcus): Known for causing outbreaks, particularly in crowded settings like college dorms. This bacterium can also lead to sepsis (blood poisoning). The reference context states that pneumococcal and meningococcal bacteria account for approximately 85% of bacterial meningitis cases.
*
Haemophilus influenzae type b (Hib): Once a leading cause, but dramatically reduced thanks to widespread vaccination.
*
Listeria monocytogenes: More common in newborns, older adults, and individuals with weakened immune systems, often contracted through contaminated food.
Bacterial meningitis requires immediate antibiotic treatment to prevent severe complications like brain damage, hearing loss, learning disabilities, or even death.
Viral Meningitis: The More Common, Milder Form
Often referred to as aseptic meningitis, viral meningitis is generally less severe than its bacterial counterpart and usually resolves without specific treatment.
*
Enteroviruses: These are the most common cause of viral meningitis, especially during summer and fall. They spread through direct contact with an infected person or contaminated surfaces.
*
Herpes Simplex Virus (HSV): While known for causing cold sores, HSV can also lead to meningitis, though it's less common.
*
Mumps, Measles, Influenza, and West Nile Virus: These and other viruses can also occasionally trigger meningitis.
Treatment for viral meningitis is typically supportive, focusing on managing symptoms like fever and pain, and ensuring hydration.
Other, Less Common Causes
While bacterial and viral infections are the primary drivers, other factors can also lead to meningitis:
*
Fungal Meningitis: Rare and typically affects individuals with compromised immune systems (e.g., HIV/AIDS patients, those on immunosuppressants). Fungi found in soil or bird droppings are common sources.
*
Parasitic Meningitis: Extremely rare, caused by parasites, often through contaminated food or water.
*
Non-Infectious Meningitis: In some cases, meningitis can be caused by certain drugs, autoimmune diseases (like lupus or sarcoidosis), or even specific types of cancer.
Understanding the spectrum of causes helps healthcare providers accurately diagnose and tailor treatment, underscoring why prompt medical evaluation is non-negotiable.
Key Symptoms: What to Look Out For
Recognizing the symptoms of meningitis can be challenging, as they can mimic those of the flu or other common illnesses. However, the rapid progression and the combination of specific signs should raise immediate red flags. The symptoms can vary depending on the patient's age and the cause of the infection.
Here are the critical symptoms to watch for:
*
Severe Headaches: Often described as unusually intense and persistent, unlike typical tension headaches.
*
High Fever: A sudden onset of a high temperature, often accompanied by chills.
*
Stiff Neck (Nuchal Rigidity): Difficulty or inability to flex the neck forward and touch the chin to the chest. This is a classic sign, especially in bacterial meningitis, due to the inflammation of the meninges.
*
Light Sensitivity (Photophobia): Discomfort or pain when exposed to bright lights.
*
Nausea or Vomiting: Often accompanying the headache and fever.
*
Confusion or Difficulty Concentrating: Mental fogginess, disorientation, or an altered mental state. In severe cases, this can progress to lethargy or unresponsiveness.
*
Seizures: A serious neurological symptom indicating significant irritation of the brain.
*
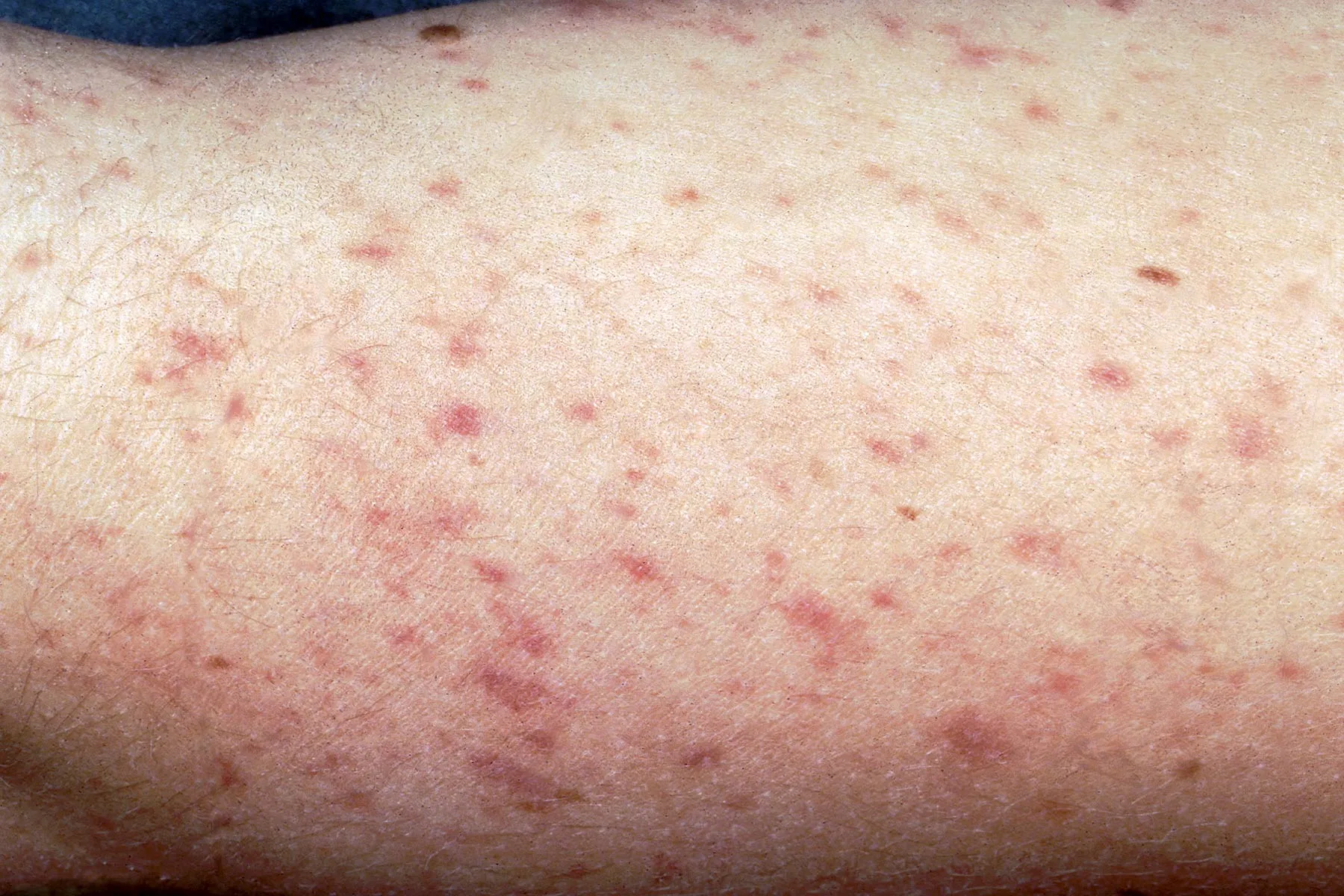
Skin Rash: Particularly with meningococcal meningitis (a bacterial form), a distinctive purplish-red or reddish-brown rash that does not fade when a glass is pressed against it (the "glass test") can appear. This is a sign of blood poisoning (sepsis) and is a medical emergency.
Symptoms in Infants and Young Children
Recognizing meningitis in infants can be particularly difficult because they may not display the classic symptoms like stiff neck or headache. Parents and caregivers should look for:
*
Irritability or Excessive Crying: Especially if accompanied by a high-pitched cry.
*
Poor Feeding: Refusal to eat or drink.
*
Lethargy or Sleepiness: Difficulty waking the baby, or the baby being unusually floppy.
*
Bulging Soft Spot (Fontanelle): The soft spot on a baby's head may appear swollen.
*
Body Stiffness or Floppiness: Unusual posture or movements.
*
Fever: Though sometimes the baby's temperature might be lower than normal.
Any combination of these symptoms in an infant warrants immediate medical evaluation.
For a deeper dive into the symptoms and treatment pathways, see
Meningitis Explained: Causes, Symptoms, and Urgent Treatment.
Why Early Action Matters: The Urgency of Medical Intervention
The single most critical piece of advice regarding meningitis is this:
if you suspect meningitis, seek immediate medical attention. Early diagnosis and prompt treatment are not just important; they are absolutely crucial for preventing severe complications and saving lives.
Consider the following points:
1.
Rapid Progression: Bacterial meningitis, especially, can worsen extremely quickly. What starts as a mild headache can escalate to a life-threatening condition within hours.
2.
Preventing Complications: Delayed treatment significantly increases the risk of serious, long-term complications. These can include:
*
Brain damage: Leading to cognitive impairments, learning difficulties, or developmental delays.
*
Hearing loss: Partial or complete.
*
Seizures and epilepsy.
*
Loss of limbs: In severe cases of sepsis associated with meningococcal disease.
*
Death: Despite modern medicine, meningitis can still be fatal, particularly bacterial forms.
3.
Targeted Treatment: Early diagnosis allows healthcare professionals to determine the specific cause (bacterial, viral, fungal) and initiate the most effective treatment. Bacterial meningitis requires potent antibiotics, which are ineffective against viral forms. Conversely, misdiagnosing bacterial meningitis as viral can have catastrophic consequences.
4.
Diagnostic Process: Diagnosing meningitis typically involves a physical examination, blood tests, and often a lumbar puncture (spinal tap) to analyze the cerebrospinal fluid. This process takes time, and every minute counts.
The reference context emphasizes that "vroege diagnose en behandeling zijn cruciaal om complicaties zoals hersenschade of zelfs overlijden te voorkomen." This translates directly to the undeniable fact that prompt medical intervention is the most powerful tool we have against the devastating impact of meningitis.
Prevention and Risk Factors
While the primary focus is on early detection, understanding prevention and risk factors is equally vital.
Prevention Strategies:
*
Vaccination: Vaccines are highly effective against several common causes of bacterial meningitis, including meningococcal, pneumococcal, and Hib. Staying up-to-date with recommended vaccinations is one of the best defenses.
*
Good Hygiene: Regular hand washing, especially after coughing, sneezing, or using the restroom, can help prevent the spread of viruses and bacteria. Covering your mouth and nose when coughing or sneezing also reduces transmission.
*
Avoid Sharing: Do not share eating utensils, drinking glasses, or personal items that come into contact with saliva.
Risk Factors:
Certain individuals are at a higher risk of developing meningitis:
*
Age: Infants, young children, and adolescents are particularly vulnerable. Older adults also face increased risk.
*
Community Living: People living in close quarters, such as college students in dorms, military recruits, or children in childcare centers, have a higher risk of contracting infectious forms of meningitis.
*
Compromised Immune System: Individuals with weakened immune systems due to conditions like HIV/AIDS, cancer treatment, or organ transplants are more susceptible, especially to fungal meningitis.
*
Certain Medical Conditions: Conditions like sickle cell disease, removal of the spleen, or a cochlear implant can increase risk.
*
Unvaccinated Individuals: Those not vaccinated against the common bacterial pathogens are at higher risk.
Conclusion
The
Meningitis Betekenis extends far beyond a simple definition; it encompasses a severe health threat demanding vigilance and swift action. Recognizing the key symptoms—severe headache, fever, stiff neck, light sensitivity, and confusion—is paramount, especially given their potential to mimic less serious illnesses. While the causes of meningitis are diverse, ranging from bacterial to viral and even fungal, the need for immediate medical evaluation upon suspicion remains constant. Early diagnosis and prompt, appropriate treatment are not merely recommended but are absolutely critical to preventing long-term neurological damage, hearing loss, and ultimately, saving lives. By staying informed, practicing good hygiene, ensuring vaccination, and acting decisively at the first sign of concern, we can collectively reduce the devastating impact of this serious condition. Never hesitate to seek emergency medical care if you suspect meningitis—it could make all the difference.