Meningitis Causes: Understanding Bacterial, Viral, and Prevention
Meningitis is a serious and potentially life-threatening condition that involves the inflammation of the protective membranes surrounding the brain and spinal cord, collectively known as the meninges. This inflammation also affects the cerebrospinal fluid (CSF) that bathes these vital structures. When we talk about Meningitis Explained: Causes, Symptoms, and Urgent Treatment, it's crucial to grasp that while many factors can trigger this inflammation, the primary culprits are often infections – particularly bacterial and viral pathogens. Understanding the underlying causes is paramount for accurate diagnosis, effective treatment, and crucially, prevention.
What is Meningitis? Unpacking the "Meningitis Betekenis"
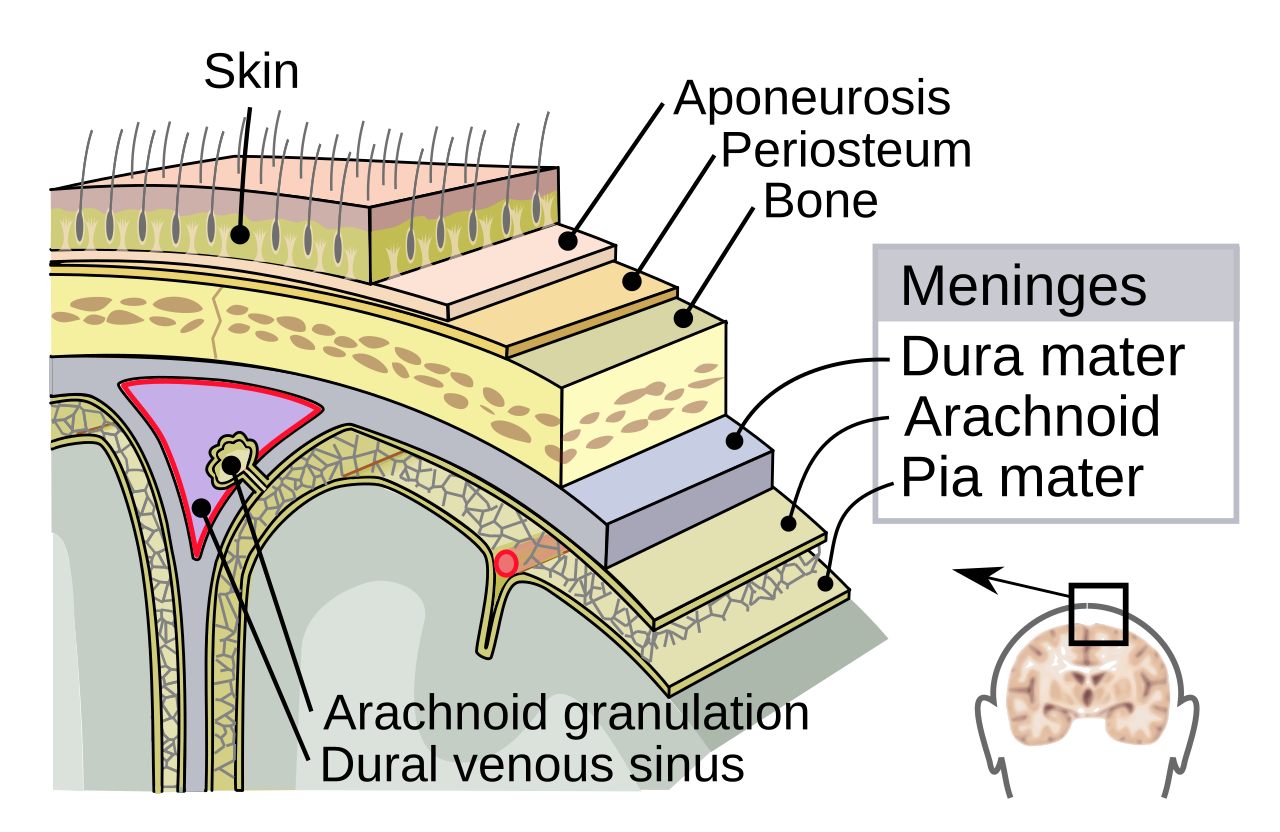
The term "Meningitis Betekenis" translates directly to "Meningitis Meaning," and its meaning points to a critical medical condition. Essentially, it signifies an inflammation of the meninges, the three layers of membrane (dura mater, arachnoid mater, and pia mater) that protect the delicate brain and spinal cord. This inflammation can cause swelling and pressure, leading to a cascade of severe symptoms that demand immediate medical attention. Without prompt treatment, meningitis can lead to devastating complications such as brain damage, hearing loss, seizures, or even death. The rapid onset and potential severity make early recognition and intervention absolutely vital.
The Primary Causes of Meningitis: Bacterial, Viral, and More
Meningitis is not a single disease but rather a syndrome that can be triggered by various agents. The most common infectious causes are bacteria and viruses, though fungi, parasites, and even non-infectious conditions can also play a role.
Bacterial Meningitis: A Serious Threat
Bacterial meningitis is often regarded as the most dangerous form due to its rapid progression and potential for severe, long-term complications or fatality if not treated promptly. It is a rare but extremely serious illness. Common bacteria responsible for this form include:
- Streptococcus pneumoniae (Pneumococcus): This bacterium is a leading cause of bacterial meningitis in infants and young children, as well as adults. It can also cause pneumonia, ear infections, and sinusitis.
- Neisseria meningitidis (Meningococcus): Known for causing meningococcal meningitis, this bacterium is particularly concerning in crowded community settings like dormitories, military barracks, and schools. It can spread quickly and sometimes causes a characteristic rash.
- Haemophilus influenzae type b (Hib): Once a very common cause, its incidence has drastically reduced in countries with routine Hib vaccination programs.
- Listeria monocytogenes: This bacterium primarily affects newborns, pregnant women, older adults, and individuals with weakened immune systems. It is often linked to contaminated food.
- Group B Streptococcus: A common cause of meningitis in newborns, acquired from the mother during birth.
These bacteria often reside harmlessly in the nose and throat of many individuals. However, if they enter the bloodstream and travel to the brain and spinal cord, they can trigger a severe infection. The body's immune response to this invasion leads to the inflammation characteristic of meningitis. The urgency of bacterial meningitis treatment cannot be overstated; antibiotics are crucial and must be administered without delay.
Viral Meningitis: The More Common, Milder Form
Viral meningitis is far more common than its bacterial counterpart and, while still serious, generally causes a milder illness. It usually resolves on its own without specific treatment. The viruses most frequently responsible include:
- Enteroviruses: These are the most common cause of viral meningitis, especially during summer and fall. They can spread through respiratory droplets or contact with contaminated surfaces.
- Herpes Simplex Virus (HSV): While typically associated with cold sores or genital herpes, HSV can, in rare cases, cause meningitis.
- Mumps Virus: Before routine vaccination, mumps was a common cause of viral meningitis.
- Measles Virus: Similar to mumps, measles can also lead to meningitis, though less frequently due to widespread vaccination.
- Arboviruses: Viruses transmitted by mosquitoes or ticks, such as West Nile virus or La Crosse encephalitis virus.
- HIV: Human Immunodeficiency Virus can also be a cause of meningitis, particularly during the acute phase of infection.
Viral meningitis typically spreads through respiratory droplets from coughing or sneezing, or through contact with feces of an infected person (especially with enteroviruses). Good hygiene practices are vital in preventing its spread.
Less Common Causes: Fungal, Parasitic, and Non-Infectious
While less frequent, other agents can also cause meningitis:
- Fungal Meningitis: This is relatively rare and primarily affects individuals with compromised immune systems (e.g., those with HIV/AIDS, cancer, or on immunosuppressant drugs). Fungi like Cryptococcus neoformans, often found in soil contaminated with bird droppings, or Coccidioides (valley fever fungus) can cause this type.
- Parasitic Meningitis: Extremely rare, this can be caused by parasites such as Naegleria fowleri (an amoeba found in warm freshwater).
- Non-Infectious Meningitis: In some cases, meningitis can result from non-infectious conditions, including certain cancers (carcinomatous meningitis), autoimmune diseases (e.g., lupus), certain medications (e.g., some NSAIDs, IVIG), head injuries, or brain surgery.
Risk Factors for Meningitis: Who is Most Vulnerable?
Understanding the risk factors associated with meningitis is crucial for prevention and early detection. While anyone can develop meningitis, certain groups are more susceptible:
- Age: Infants (especially newborns) are at higher risk for bacterial meningitis due to their underdeveloped immune systems. Adolescents and young adults (16-23 years) are also at increased risk for meningococcal meningitis, particularly if living in close quarters like college dorms.
- Weakened Immune System: Individuals with compromised immunity due to conditions like HIV/AIDS, cancer, organ transplantation, or certain medications are more vulnerable to various forms of meningitis, especially fungal.
- Community Living: Spending time in close quarters, such as dormitories, boarding schools, or military barracks, increases the risk of meningococcal meningitis due to easier transmission of respiratory droplets.
- Certain Medical Conditions: People with a damaged or absent spleen, or those with specific genetic immune deficiencies, have a higher risk. Cochlear implants have also been linked to an increased risk of pneumococcal meningitis.
- Travel: Traveling to certain regions (e.g., the meningitis belt in sub-Saharan Africa during dry seasons) can increase exposure to specific pathogens.
- Contact with Farm Animals/Soil: Certain bacteria and fungi linked to meningitis can be found in animal waste or soil.
Maintaining good overall health and a strong immune system can help reduce general susceptibility to infections, though it doesn't eliminate the risk entirely.
Prevention is Key: Safeguarding Against Meningitis
While not all forms of meningitis are preventable, significant strides have been made, especially against bacterial types, through vaccination and good public health practices. Here are key prevention strategies:
- Vaccination: This is the most effective way to prevent certain types of bacterial meningitis.
- Meningococcal Vaccines: Protect against Neisseria meningitidis. There are different types of vaccines for different serogroups (e.g., MenACWY, MenB). These are particularly recommended for adolescents, college students, and travelers to high-risk areas.
- Pneumococcal Vaccines: Protect against Streptococcus pneumoniae. These are recommended for infants, young children, older adults, and individuals with certain chronic health conditions.
- Hib Vaccine: Protects against Haemophilus influenzae type b and is a routine childhood immunization.
- MMR Vaccine: Protects against Measles, Mumps, and Rubella, which can prevent viral meningitis caused by these specific viruses.
- Varicella (Chickenpox) Vaccine: Can prevent meningitis in rare cases where the varicella-zoster virus is the cause.
It's important to discuss vaccination schedules with your healthcare provider to ensure you and your family are adequately protected.
- Good Hygiene Practices: These are crucial for preventing the spread of many infectious agents, especially viruses.
- Hand Washing: Wash hands frequently and thoroughly with soap and water, especially after coughing, sneezing, using the bathroom, or before eating.
- Covering Coughs and Sneezes: Use a tissue or your elbow to cover your mouth and nose to prevent the spread of respiratory droplets.
- Avoid Close Contact: Try to avoid close contact with sick individuals, particularly if they have a respiratory illness.
- Do Not Share: Avoid sharing eating utensils, drinking glasses, lip balm, or other personal items.
- Healthy Lifestyle: A balanced diet, regular exercise, and adequate sleep can help support a robust immune system, making you less susceptible to infections in general.
- Food Safety: Pregnant women and individuals with weakened immune systems should be particularly careful about food safety to prevent Listeria infection.
Despite preventive measures, meningitis can still occur. Therefore, knowing the symptoms and acting quickly is paramount. For a comprehensive overview of symptoms and why immediate action is critical, refer to our article on Spotting Meningitis: Key Symptoms & Why Early Action Matters.
Conclusion
Meningitis is a serious condition with various causes, primarily bacterial and viral infections, but also fungal, parasitic, and non-infectious factors. Understanding the "Meningitis Betekenis" – its definition, diverse origins, and the critical need for prompt action – empowers individuals to take proactive steps for prevention and recognize early warning signs. While bacterial meningitis demands urgent antibiotic treatment, viral forms typically resolve on their own. Vaccination remains the cornerstone of prevention for many severe bacterial types, complemented by diligent hygiene and a healthy lifestyle. If you suspect meningitis in yourself or someone else, do not delay; seek immediate medical attention. Early diagnosis and treatment are the best defenses against the potentially devastating consequences of this inflammatory brain and spinal cord condition.